5 ways to keep up with dental health during COVID times
by Megan Marolf | Oct 20, 2020 | homecare, seniors coping with coronavirus, senior health | 0 Comments

We might be past the stage of trick-or-treating, but we can still have unhealthy habits when it comes to our teeth. Whether that’s forgetting to brush your teeth regularly, skipping dentist appointments, or eating too much sugar, we’ve all been guilty of neglecting oral hygiene at some point.
Oral health is especially important for seniors and can signal if your overall health is off-kilter. At a time when going to the dentist and doctor regularly comes with risk, read on to find out how to keep your dental health in check.
Caring for your teeth during covid
In the days after COVID-19 was declared a pandemic, a survey from the American Dental Association found that only 5 percent of dental clinics remained open.
The ADA website recommends routine care, but also advises people to follow state closures if there are any. Throughout the pandemic until more recently, The ADA and other dental associations recommended dentists to treat for emergency services only.
According to the CDC, older adults are part of the population most vulnerable to contracting COVID-19 and are also more at risk for oral disease. People from minority populations are especially at risk during the pandemic and also have the poorest oral health.
At this point, it’s easy to be confused whether or not going to the dentist is worth the risk.
National Geographic has a guide on how to visit the dentist the safest way, such as making sure your dentist is taking extra precautions. This includes screening you for symptoms of COVID-19 before you even step into the dentist office.
Common oral health problems
Regular check ups are especially important for those who were or are currently regular smokers, or chewed tobacco in the past. These visits can detect early signs of oral cancer or alert your dentist to any health problems.
Living with a disability, being homebound or living in a nursing home are all factors of risk factors of poor dental health.
Symptoms of oral health problems to look out for according to the CDC include:
- Dry mouth- several types of medicines can affect dry mouth, and it’s also a side-effect of cancer treatment
- Gum disease- caused by a number of factors, such as smoking history, diet and other disease
- Root decay
- Receding gums
- Chronic bad breath
The median age for getting an oral cancer diagnosis is 62, which makes for a good reason to see the dentist for the recommended once a year visit at the very least.
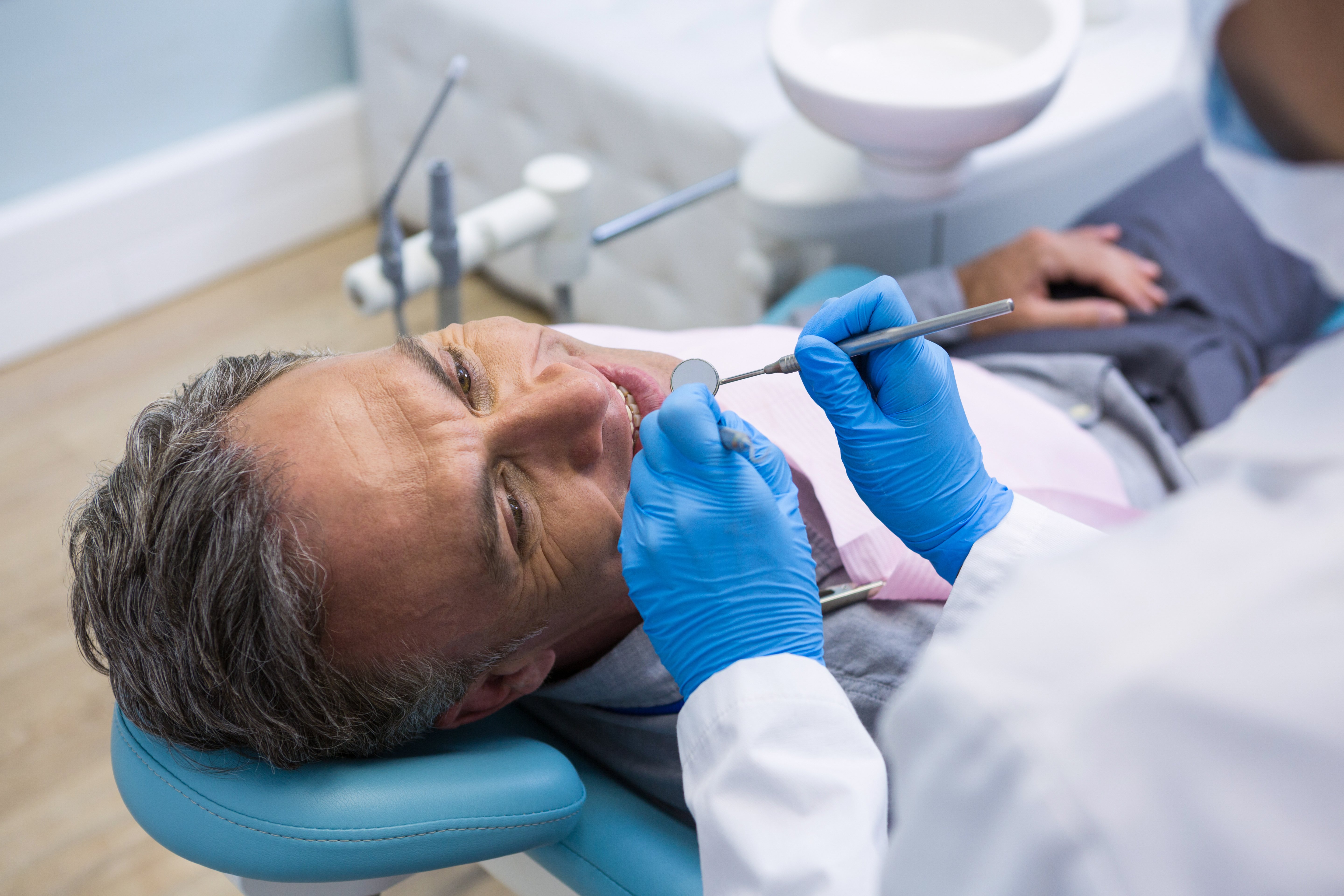
Maintaining oral hygiene and nutrition for seniors without teeth
For those with dentures, getting adequate nutrition can be a challenge. People without teeth prefer eating soft foods over crunchier ones like vegetables.
A study cited by the Geriatric Dietician found that people who ate regularly without their dentures had the lowest quality of diet. Because of this, it’s recommended that those with dentures don’t take them out when eating.
For adults with trouble chewing, soft proteins like eggs, tuna or other cooked fish can be incorporated into the diet. Smoothies can be a great source of your daily fruit serving, and soups when it comes to eating the recommended amount of vegetables.
Full or partial dentures should be removed every day for cleaning, according to the Geriatric Dietician. Bacteria can still stick to the gums like it does to teeth. The Geriatric Dietician recommends brushing the roof and tongue of your mouth in addition to rising and gently brushing your dentures.
Even for those without teeth, it’s important to get dental check-ups regularly in order to get screened for overall health and oral cancer.
Eating for oral health
Dental health affects nutrition in the elderly in many ways. The side effects of medication, diminished taste or a poor appetite can make eating seem more like a chore than an enjoyable part of daily life. And for someone with mouth or teeth issues, eating can even be painful.
Eating a diet low in sugar is a given, but what else can you do?
The Geriatric Dietician recommends a diet including phosphorus, calcium and vitamin D, which is easier than you might think.
Phosphorus is an essential mineral, according to Healthline. Most people meet the minimum requirements of phosphorus since it’s found in turkey, chicken, seafood and dairy.
Calcium can be found in the usual suspects- dairy products. For those who try to avoid dairy, you can get calcium from leafy greens such as kale and collard greens and beans and lentils
As for foods with high amounts of Vitamin D, most of those sources come from the sea. Salmon and cod oils are some examples. For vegetarians, you can get vitamin D from mushrooms.
How your caregiver can help
A caregiver can keep you on track with appointments, notice any changes to your oral hygiene or health and remind you to brush your teeth.
In case anyone forgot or has been slacking- you should be cleaning those teeth twice a day. Brushing with a soft or electric toothbrush can make the task easier for people with arthritis. Flossing at least once a day should also be part of the routine.
If you’re on a fixed income, your caregiver can help you find an assistance program by calling the local dental society, according to Web MD.
A lack of dental hygiene may be a sign that your loved one needs assistance in their daily activities. In-home care is the best option out there, at least in our opinion. Reach out to a SeaCare professional to find out what might work for you.


0 Comments