Advance directive: What is it and why do you need one?

Talking about death is rarely a pleasant conversation, especially when we’re young and in good health.
Something happens to our perception of death as we get closer to the end of our life – we accept that it’s going to happen and we begin to prepare for it. Psychologist Laura Carstensen advises that as we reach old age and recognize our time is growing shorter, we’re more apt to embrace life’s pleasures and find joy in our days.
With this mindset we’re in a good place to do advance care planning – a process that includes documenting our preferences for medical care in the event we can no longer make decisions for ourselves.
A key component of this process is the advance directive, a legal document that makes end-of-life care wishes clear. The aim of it is to ensure medical care that’s aligned with our personal values and goals. It’s a thoughtful preparation – a set of instructions that makes sense to us – to share with our loved ones.
What an excellent way to plan for the inevitable as we age and to meet our final days on our own terms.
But the National Institutes of Health (NIH) reports that just over 42% of older adults and only 1 out of 3 in the general US population have completed an advance directive. Why don’t more of us have one?
According to the NIH, lack of awareness is the reason most cited for not having an advance directive. Some are reluctant to specify treatment preferences because they fear not receiving any care if they indicate they don’t want lifesaving measures. And for others, it’s difficult to make decisions about future care when there are so many unknowns in the equation.
To be sure, there are both practical and emotional challenges to creating this important document. Let’s have a look at what an advance directive is along with good reasons to have one.
What is an advance directive?
Simply stated, an advance directive is one part of the advance care planning process, which also includes non-healthcare-related documents – a will, a durable power of attorney for finances, and a revocable living trust – as shown below. The non-healthcare components are important things to consider but are not discussed further in this article. Our focus is the advance directive.
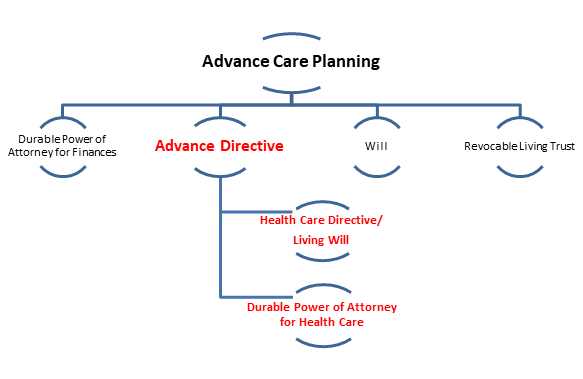
Here’s a brief glossary to help you understand how an advance directive fits into the overall process:
Advance Care Planning refers to the overall process of learning about end-of-life choices, thinking about your preferences, communicating your wishes to your family and health care providers, and preparing documentation that reflects your decisions.
An Advance Directive is a legal document that goes into effect if you are not able to speak for yourself. It describes the health care choices you made before you became incapacitated about your wishes for life-sustaining treatment. It requires you to name a health care agent to act on your behalf – someone to make the difficult decisions you are unable to make, such as whether you do or do not want resuscitation, the use of an artificial ventilator, and artificial nutrition and hydration.
A Health Care Directive (also known as a Living Will) is a type of advance directive that becomes effective as end-of-life guidance. It specifies what you want and what you don’t want. It does not require the naming of a health care agent, which could cause some indecision if your health care providers encounter a situation that isn’t spelled out in the document.
A Durable Power of Attorney for Health Care (DPOAHC) is another type of advance directive that requires you to name a health care agent who is authorized to make care decisions on your behalf.
A Health Care Agent is a trusted friend or family member you designate to make decisions about your medical care in the event you can no longer speak for yourself.
For our purposes in Washington State, the End of Life Washington organization has combined the Health Care Directive and the Durable Power of Attorney for Health Care into a single document that’s accepted by health care professionals and elder care attorneys as a comprehensive and legally binding document. The link takes you to sample advance directive forms.
Why do you need an advance directive?

Death is a certainty with an uncertain timeline. Even though we can’t predict the end of our life, we can take steps to prepare for it.
An advance directive is good preparation for the unexpected. While life-threatening injury or illness can happen to anyone, older adults are more vulnerable. If it happens that you are no longer able to speak for yourself and make decisions about your care, your health care agent is able to act for you with instructions from the advance directive.
Creating an advance directive is being proactive about your health. The process helps you think about quality of life and what that means to you. For example, imagine the prospect of being permanently bedridden and completely unable to care for yourself or fully dependent on an artificial ventilator. If this were the case, would you want resuscitation in the event your heart or breathing stopped?
Advance directives provide guidance to your loved ones and your health care providers. The family and providers who care for you have the assurance of your documented wishes if they face difficult decisions. Maybe your preference is for pain relief and comfort – also known as palliative care. Or you may want providers to intervene with more aggressive, life-prolonging medical treatments.
Appointing a health care agent in your advance directive means your trusted loved one can speak with your medical provider. Your medical privacy is protected by Federal law (HIPAA – the Health Insurance Portability and Accountability Act), and without a health care agent, even your closest family member may not be able to advocate for your wishes with providers and hospital staff. Your advance directive explains your wishes and names the person responsible for making decisions on your behalf.
Making an advance directive can be done at no cost. It’s a relatively easy, step-by-step process, although you’ll want to take some time with your choices. Make a draft plan, let it sit for a while, and then discuss it with the person you’ve chosen as your health care agent before finalizing it. Rest assured you can amend it if necessary, particularly if you experience a significant change in your health and plans for treatment. The ideal time to make your advance directive is while your health is still stable.
Your advance directive is a legal document. When you share it with your health care provider it becomes part of your medical record, which means it’s readily available to hospital staff. Your chosen health care agent and immediate family members should also have copies.
Creating an advance directive is an opportunity to talk frankly with your loved ones about the way you want to live the rest of your life. You’ll be thinking about the future, imagining what your life will be like, and examining your priorities for your final days. It’s the perfect time to share your thoughts with your immediate family. The topic might sound grim, but you’ll likely discover that by starting the process you’ll experience satisfaction in knowing you have a plan in place. It’s a gift you offer your loved ones and yourself.
If you’d like to learn more, A Beginner’s Guide to the End: Practical Advice for Living Life and Facing Death by BJ Miller, MD, and Shoshana Berger provides readable, humorous, and comprehensive guidance. It’s available through the King County Library and Seattle Public Library systems.
SeaCare has published a follow-on article HERE about the emotional challenges you may face while doing advance care planning. It includes steps to putting your wishes on record and how to have conversations with your family about it.
The staff at SeaCare understands the sensitive nature of thinking about the final chapter of life. Ask us about in-home care and support for you and your loved ones.
Katie Wright writes about aging and senior wellness from Bellingham, WA. You can read more about her here.
References:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6345507/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4540332/
{{cta(‘b0886078-d0f4-4325-933f-620bf9cdd921’)}}

